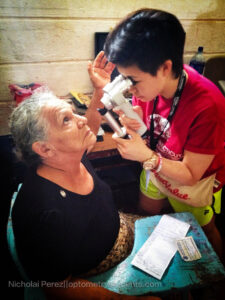
This past January, I had the wonderful opportunity to conduct eye exams at the annual eye care clinic with VOSH-Connecticut in Nicaragua. Twenty-one optometry students from Berkeley Optometry joined a team of eight optometrists and 24 additional volunteers to serve the beach town of San Juan Del Sur and its neighboring communities. Over four days at the elementary school Centro Escolar Enmanuel Mongalo y Rubio, our clinic saw 3,129 patients! Many patients traveled long distances from neighboring towns like Rivas, San Jorge, and Masatepe to receive eyecare. For many, our clinic was their only access to any sort of vision care. During the trip, I compiled a list of 13 things anyone who wants to go on a mission trip must know to have a successful trip:

1. Learn simple key phrases in the local language. Even if you have a translator available, just knowing a few phrases will make your life much easier. Previously, my Spanish training was nil (unless you count the menu at the taqueria on Mission St. in San Francisco). Aside from the case history and consultation, I was pretty much able to successfully conduct eye exams using these phrases with patients who spoke no English over my four days of clinic. Of course, using a lot of gestures, facial expressions, and intonations to convey meaning made up for my very broken Spanish. The key phrases that you absolutely need to know are:
- “Look over there” or “Look at the big E.” This is a useful phrase for retinoscopy or direct ophthalmoscopy.
- “Please read line 4.” Or Line 5. Or Line 6. This phrase is extremely useful in checking VA’s.
- “Which is better, one or two?” Refraction, duh.
- You absolutely need to know how to translate “Blurry” and “Clear”. You, yourself, won’t be using those words as often during your exam, but patients will definitely let you know when something is blurry. But if they tell you everything is clear, you know you’ve just rocked that refraction.
And there you have it. You can now go conduct an eye exam in any part of the world! If you ever run into difficulty communicating to your patient, just call for your translator.
2. Be familiar with the prevalent diseases in that country or demographic. In countries near the
 equator like Nicaragua, incidences of pterygiums and pingueculas are much higher. Also, presbyopia occurs at a much earlier age, so you’d be prescribing higher adds for a younger population compared to what you’re used to in the U.S. In addition, we saw a lot of against-the-rule astigmats and hyperopes, and only a few myopes. On the other hand, perhaps in Asian countries, the prevalence of myopia would be much higher. As long as you do some research on the conditions in the region of your clinic, you would be prepared for it when it comes.
equator like Nicaragua, incidences of pterygiums and pingueculas are much higher. Also, presbyopia occurs at a much earlier age, so you’d be prescribing higher adds for a younger population compared to what you’re used to in the U.S. In addition, we saw a lot of against-the-rule astigmats and hyperopes, and only a few myopes. On the other hand, perhaps in Asian countries, the prevalence of myopia would be much higher. As long as you do some research on the conditions in the region of your clinic, you would be prepared for it when it comes.
3. Most of the time, if you can get their VA down to 20/30, you have done your job. You may not be able to refract all the way to 20/20 or 20/15, and that’s okay. You might think that you’re cheating them of their best potential vision, but in a remote clinic in an area with limited resources, 20/30 acuity is adequate. There are several reasons for this mindset:
- Think about what they do for a living. Do they need that super-human distance vision at 20/20 if the patient is a housewife or a farmer?
- If you spend all your time meticulously, painstakingly refracting the patient so they see 20/20, and the dispensary doesn’t even have a pair of glasses that match your prescription, you have just wasted 30 minutes of your time when you could have started on the next patient.
- The patient might have a pathological problem that won’t allow them to see 20/20. J
 ust try your best with your trial frame refraction to obtain their best VA, and you’re done.
ust try your best with your trial frame refraction to obtain their best VA, and you’re done.
4. Be understanding of the dispensary. They have a hard job. There are no stock or uncut lens blanks in the dispensary. Nor is there a lens edger. The dispensary operates solely on the boxes and boxes of donated glasses from Lion’s Club. For the sheer volume of glasses they have, the dispensary does very well to keep them organized by single vision vs. bifocals, plus lenses vs. minus lenses, etc. When the patient arrives with the prescription that the clinicians give them, the volunteers in the dispensary sift through the boxes and boxes of donated glasses of varying prescriptions to find something closest to the prescription we give them. It is usually extremely difficult to find something that matches the prescription exactly. The volunteers at the dispensary then choose a few pairs of glasses for the patient, which the patient may reject based on blurriness or cosmesis. This subsequently sends the dispensary volunteer back to “square one” to try to find another pair. It also helps the dispensary prioritize what kind of glasses to give to the patient if the patient favors one eye over the other (due to eye dominance, pathology, balance, etc).
5. Refract in 0.50D steps. Find your closest axis to 180°, 45°, 90°, or 135°. See #3 and #4. There is no use refracting to the nearest 0.25D or debating between axis 005 and 010 if the dispensary does not have it. Furthermore, wouldn’t the patient really appreciate that extra 0.25D of clarity based on your trial frame refraction?

6. For some people, you may want to check their fundus before you do retinoscopy or refraction. You won’t be able to refract the patient down to 20/20 if he or she has a dense cataract or macular degeneration. Per the recommendation of one of our supervising doctors, I actually started every exam with direct opthalmoscopy before retinoscopy.
7. The patient is not always reliable. Here is a short list of scenarios my colleagues and I encountered in Nicaragua that makes us pause before fully trusting the patient:
- In trial frame refraction, be wary of the glare caused by stacking lenses in front of another. The patient might choose the option with less glare.
- The patient might be biased and believe a lens is always better than no lens.
- The patient might be there only to obtain eye drops even if they don’t have symptoms of dry eye, allergy, inflammation, or any other conditions.
- The patient might be there only because they want some glasses despite not having refractive error. You can usually distinguish these patients with funky refraction results with VA. For example, they could only see the 20/400 “E” without glasses, but they moment you give them 0.25D, they can suddenly see the entire chart.
8. Be nice to everyone, especially your translators. And the lunch lady. Most likely, you won’t get your own personal translator. He or she probably has to float around the room doing the most important job of all. They are a huge asset to a successful exam and transparent communication with the patient despite a language barrier. And be nice to the lunch lady because she might sneak you an extra piece of fried chicken during lunch.
 9. Dress comfortably and appropriately. Comfortable sneakers, short-sleeve shirt, and shorts on the bottom. This is appropriate clinic attire at a mission clinic in Nicaragua. You will be on your feet, walking around, moving around, bending over, kneeling down – all day. You will be dirty, sweaty, and sticky. You want enough clothing to cover up, but not an extra layer of fabric to stick to your body in the humid weather.
9. Dress comfortably and appropriately. Comfortable sneakers, short-sleeve shirt, and shorts on the bottom. This is appropriate clinic attire at a mission clinic in Nicaragua. You will be on your feet, walking around, moving around, bending over, kneeling down – all day. You will be dirty, sweaty, and sticky. You want enough clothing to cover up, but not an extra layer of fabric to stick to your body in the humid weather.
10. Flippers are your best friends in trial frame refraction. They were so much easier to hold. They were also easier to demonstrate the plus and minus directions quickly without balancing four different trial lenses in your hands.
11. Hydrate, hydrate, hydrate. Working intensely for such long hours in humid and stuff conditions will completely drain you before you get to your fourth patient of the day. Stay hydrated to keep you refreshed throughout the day. Everyone in our clinic bought large 1-liter bottles of water at the corner market and placed them in the freezer the night before. There is nothing like icy, thirst-quenching water to get you through the day.
12. Keep your cool. There will absolutely be times when you are at a loss. Your refraction may not be producing the results you wanted. Or maybe your patient has end-stage glaucoma or severe AMD and asked you what are the chances of him having better vision with
 glasses. No matter what you’re feeling on the inside, you absolutely cannot show frustration or despair in front of your patient. Your job as a clinician, is not only to be professional, but also to be strong for your patient. This applies not only to our everyday clinic in the States, but in third-world countries where the patient has very limited resources and the situation might look more bleak. This makes it even more important for you as the clinician to be compassionate and courageous.
glasses. No matter what you’re feeling on the inside, you absolutely cannot show frustration or despair in front of your patient. Your job as a clinician, is not only to be professional, but also to be strong for your patient. This applies not only to our everyday clinic in the States, but in third-world countries where the patient has very limited resources and the situation might look more bleak. This makes it even more important for you as the clinician to be compassionate and courageous.
13. Embrace every moment as a life-changing learning experience. You will see so many things that you have never seen before. There will be trying times, and your character will be tested. Take advantage of the close proximity with the supervising doctor and ask a lot of questions.
Finally, volunteering on a mission clinic such as this one will give you a heartwarming reminder of why you do what you do. When the patient’s eyes light up (no pun intended) from finally having clear vision with the glasses you prescribed for them, it will reaffirm in you that aside from entrepreneurship, scheduling flexibility and salary, optometry is ultimately about helping people. Optometry is about fixing a system that is broken, restoring a person’s ability to capture, appreciate, and understand the world. The skills and perspectives I gained in Nicaragua will surely follow me as I continue on my journey to a career in optometry.
Don’t hesitate to share your mission trip experience or advice in the comments below!




